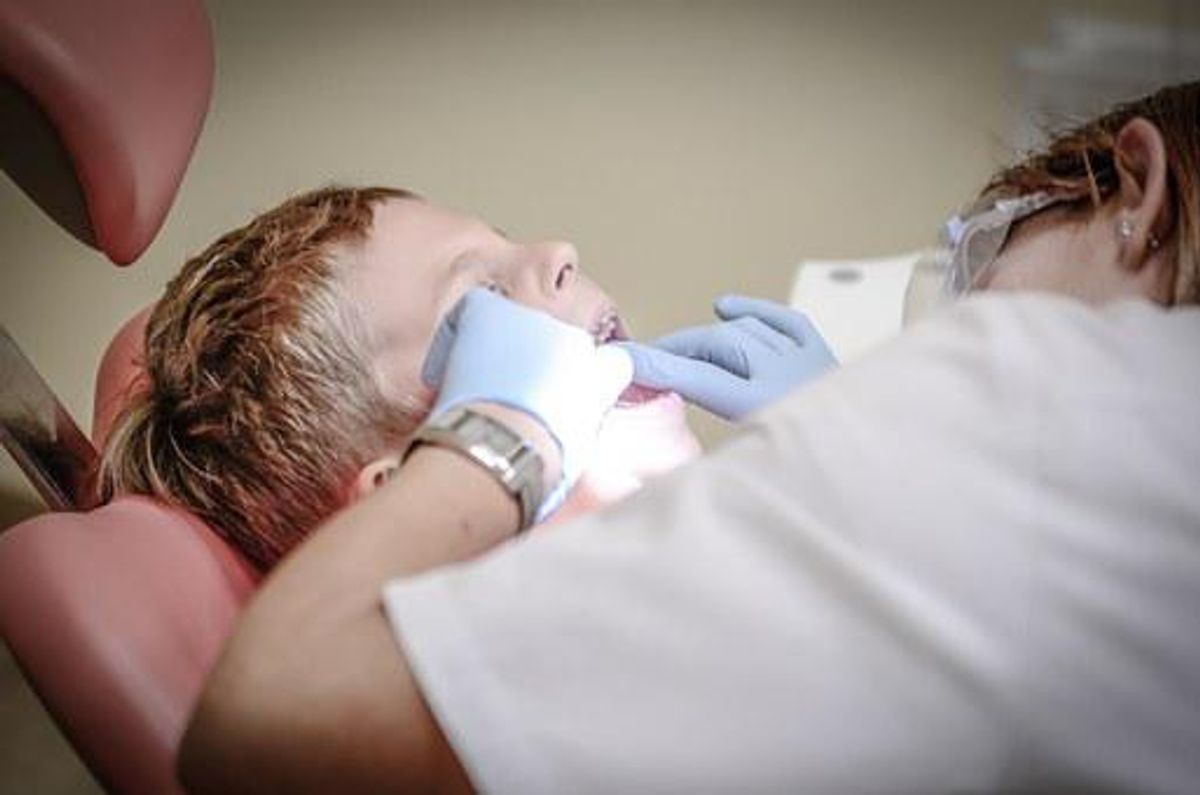
Patients unfamiliar with sleep dentistry can find it puzzling and wonder about safety. They generally don’t understand how or in case it is used in conjunction with “traditional” anesthetic approaches used in the field of dentistry. One of the most significant changes in the industry of dentistry is the option of sedation dental care – supplying the same levels of comfort which can be routinely provided by doctors regarding general medicine and relevant fields of specialty.
The particular ADA and regulatory express dental boards across the United. S. are facilitating this specific change in dentistry and helps to ensure that dentists who supply sedation dentistry do it properly. The questions and responses below are intended to help you realize both some of the history and a broader explanation of how the field of dentistry is safely being made more at ease than ever for patients.
When did dentists start using sleep?
Perhaps the better question will be, “When did dentists commence providing pharmacological pain supervision techniques? ” Horace Water Wells, a Connecticut dentist, launched the use of nitrous oxide in the 1840s. One of Wells’ pupils, William Morton, demonstrated using ether as anesthesia.
These people were progressive thought leaders within the education of pharmacological pain management because of not only in the field of dentistry but also in an area of medicine. Many, many years have elapsed since then — long enough for the effects of various sorts of anesthesia – both local and general – to become very precisely understood. Various kinds of anesthesia are the most appropriate for several types of treatment. The areas of dentistry and medication at large now have an excellent knowledge of the risks associated with all types of sedation/anesthesia.
What role does sleep play in providing comfort and ease in dentistry?
There are actually 2 issues – anxiety as well as pain – that are frequently tightly intertwined when it comes to creating patient comfortable during dental care procedures. Dentists receive a significant amount of training that helps them fully grasp this. They are taught about 2 techniques for managing both nervousness and pain – typically the psychological approach and the medicinal approach.
Most patients get little or no awareness of dentists’ information on psychological anxiety/pain management, or maybe that those techniques are actually applied to them. At best, they might think that the expert from the psychological approach is great, gentle, and caring rapid and that’s OK! Don’t be anxious, though – there’s nothing deviant about the approaches dentists make use of to make you more comfortable during your pay visit.
For many decades, the medicinal approach used by general dental practices has been centred on the management of local anesthesia (often with needles) to numb the actual affected area. With brand new, expert training programs, dental practitioners are starting to use wider approaches that nicely enhance the use of localized (more traditional) pharmacological approaches. Patients tend to be put in a relaxed condition so they don’t mind getting necessary or elective dental care procedures performed.
Sometimes this really is needed to manage patient anxiousness – including a phobia concerning the use of needles. Once the sleep is in use, the patient can become unaware of or uncaring in regards to the use of a needle which to provide localized suppression involving pain. So, expert medicinal management of pain along with anxiety involves the use of the perfect blend of sedation and local ease – as appropriate for the method being performed.
Why don’t dental practices use general anesthesia?
When general anesthesia (where the person is rendered unconscious) is employed by dentists in some career fields of dental specialty (most notably oral surgeons), the idea carries with it a considerably greater patient risk. Additionally, it requires very specialized coaching. For this reason, general anesthesia is normally administered only in a medical centre setting where a synthetic airway can be maintained in order to facilitate an instant resuscitation try.
Needless to say, the hospital setting (or equivalent investment in service, equipment, and specialized personnel members) makes it a costly choice. Oral surgeons usually recommend that lesser sedation methods be used in conjunction with local inconsiderateness whenever practical to avoid excess patient risk. Insurance coverage (or lack thereof) for applying general anesthesia for reduced procedures is another consideration.
Are available different levels of sedation dentistry?
The American Dental Association (ADA) carries a general policy that looks at minimal, moderate, and serious sedation. The policy is usually fully described in Tips for the Use of Sedation along with General Anesthesia by Dental practices. However, it is important to realize that typically the ADA does not formally get a grip on the provision of dentistry in the U. S.; the actual regulatory responsibility lies along with each individual state.
The regulating requirements for dentists who else provide sedation dental care can differ from state to state. Some states offer requirements that define more granulosa levels of sedation dental care — each with an appropriate related level of training and/or encounter – for both the dentist as well as staff members.
For example, the reasonable level might be split into mouth administered moderate sedation as well as intravenous moderate sedation. The actual latter carries with it increased patient risk. Some claims are considering or have enacted brand-new regulations for sedation dentistry because of the increased public regarding sedation dentistry.
Aren’t most general dentists trained to conduct sedation dentistry?
The state-administered regulations for sedation dental treatment (when they exist) might be in addition to whatever state recommendations currently exist for the operations of “traditional” localized sorts of anesthesia. (The use of neighbourhood anesthesia may often possibly be regulated by states by means of certifying that the practitioner supports a Doctor of Dental Surgical procedures (DDS) from an accredited tooth school, and may include many additional continuing education requirements. )
The ADA is loyal to dentists who are adequately trained in the use of minimal, mild, and deep sedation. As well as, the ADA recommends this no dentists use prescription drugs or techniques for which they haven’t been appropriately trained.
Through the U. S., there is schooling on sedation dental care readily available through pre-doctoral, post-graduate, move-on, and continuing education programs that could be appropriate for some levels of insertion. Again, each state becomes what training and qualification procedures are appropriate for cosmetic dentists practising in the state: including sedation dentistry.
The particular ADA indicates that strong sedation and general inconsiderateness training are beyond the particular scope of either pre-doctoral or continuing education training plans. Check with the state dental table for your state for additional information about sleep dentistry regulations that connect with you and your dentist.
Read also: Precisely what is Medical Negligence?