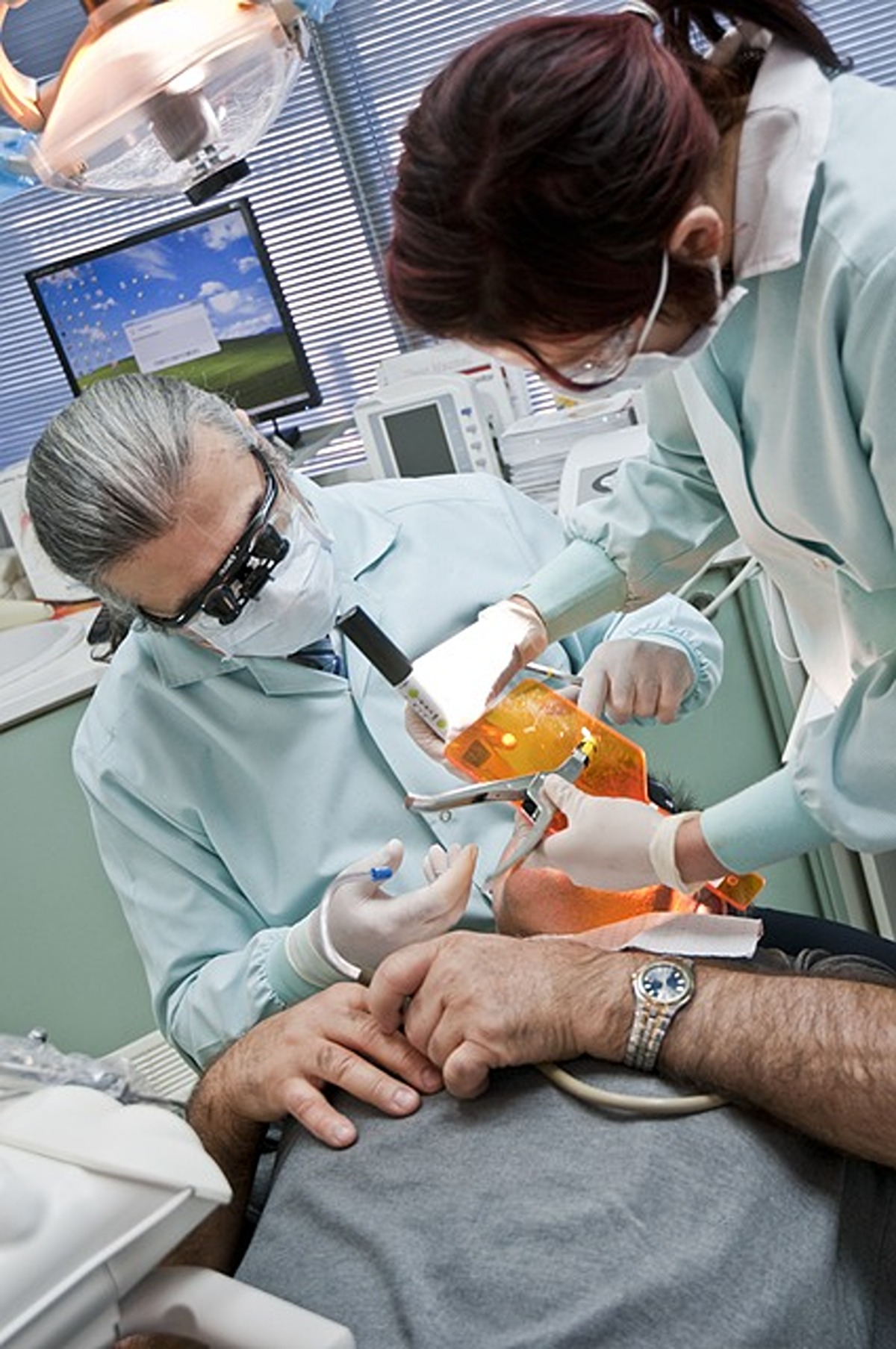
Whenever experiencing any dental emergency, it’s wise to seek treatment from an emergency dentist near me immediately. Even seemingly minor issues can quickly become more severe if left unattended. Find out the best info about Zahnarzt Bern.
Dental emergencies may include painful tooth sensitivity, bleeding gums, infection, or cracked teeth. Emergency dentistry services treat dental trauma quickly to relieve pain while protecting against further infection or treatment requirements.
Toothache
As soon as you experience oral pain or discomfort, it’s vitally important that you seek medical advice immediately. Doing so can prevent further aggravation of symptoms and potential signs of severe medical conditions or injuries that must be treated immediately.
Toothaches occur when something is wrong with one or more teeth or their surrounding tissue, including tooth decay, infection, or damage to a dental restoration. Pain associated with this issue may range from mild to severe and be constant or intermittent.
If you are experiencing tooth pain, make an appointment with an emergency dentist immediately. Be sure to bring any symptoms you are experiencing along with you; this will enable them to accurately diagnose the source of pain and provide appropriate treatment options.
If you can’t reach your regular dentist for any reason, many urgent care clinics have dental providers on staff who can address dental emergencies. These providers can often treat cracked or broken teeth, painful jaws, and swallowed or loosening teeth and prescribe antibiotics if an infection exists; such infections may even spread to other parts of the body and be life-threatening in some instances.
Chipped or Broken Teeth
Dental injuries can happen at any time and in any circumstance – whether from falling, receiving a blow to the mouth, or chewing something hard enough for them to crack and break. While chipped or broken teeth may be painful, they must be treated promptly to prevent further damage and infections.
Cracked teeth may vary from small cosmetic cracks, known as “craze lines,” that only affect the enamel to deeper apertures extending into its root structure. Treatment will depend on the extent and depth of damage and whether any nerves may be involved.
Chipped teeth may result from trauma, tooth decay, poor brushing practices, or opening bottles with your teeth. To prevent chipped or broken teeth from happening in the first place, wear a mouthguard when participating in sports or recreational activities and refrain from chewing hard and crunchy foods like ice or popcorn kernels.
If you experience a chipped tooth, rinse your mouth with warm water and apply pressure with gauze or damp tea bags (tannic acid from tea can help the blood clot more quickly). If possible, save any broken pieces of tooth to bring to the dentist for repairs; over-the-counter pain relievers such as ibuprofen or acetaminophen may help alleviate discomfort until then.
Broken Jaw
An injury to the jaw can be an urgent dental emergency and must be treated promptly. Signs of such damage include swelling, teeth that don’t fit together correctly, difficulty opening and closing your mouth, or an inability for the jaw to move. You might experience dull or sharp pain that worsens over time or an audible click when opening your mouth.
If you suspect you have a broken jaw, contact a 24-hour dentist and describe your symptoms. They’ll perform a physical exam and X-rays to accurately view injuries sustained and help find appropriate specialists, such as facial plastic and reconstructive surgeons or oral surgeons.
While waiting to be seen, apply ice to reduce swelling and pain in your injured area. If your jaw has dislocated, manually hold it into place until reaching medical care – self-correction could do more damage. A cup should also be handy to collect any drool or blood until medical help arrives. Surgery may be required for severe injuries where metal plates or bars will be attached to hold broken parts together while the bone heals – contact an orthopedic doctor as soon as possible for repair services.
Tooth Extraction
Tooth damage may become too extensive to be repaired with crowns or fillings, necessitating an extraction procedure. A dental clinic or hospital may perform the extraction with local anesthesia to numb the area before starting so the patient doesn’t experience pain during or after the process. They’ll also ask the person about any medical conditions that increase the risk associated with surgery, such as pregnancy and preexisting conditions that increase complications from extraction surgery.
Once a tooth has been extracted, a dentist or oral surgeon may apply gauze over the extraction site and request that their patient bite down with firm pressure to stop bleeding and help form a blood clot. They then remove this gauze once the bleeding has subsided – some light bleeding may still occur over 24 hours afterward.
Avoid placing pressure or irritating the area using straws, vigorous brushing, or forcibly spitting out water, as this can lead to dry socket syndrome – an excruciating pain caused by bone exposure due to no blood clot covering it. For best results, use antimicrobial mouthwash twice daily while brushing other parts of your mouth using soft toothbrushes.
Read Also: Randm Tornado 7000 Puff: A Quantum Leap in Vaping Technology